Samuel Bonnet:
the most vulnerable communities
Samuel Bonnet, LF’18, has been senior advisor to the director-general of the International Committee of the Red Cross (ICRC) since 2018. Prior to his Loeb year, Samuel was head of construction for the ICRC and led large scale health infrastructure projects in more than 20 countries affected by armed conflicts and/or natural disasters. He spoke about how his work has changed during the pandemic to a Loeb community gathering in April.
Mogadishu Keysaney Hospital operating theatre, 2012. Photo: S. N.
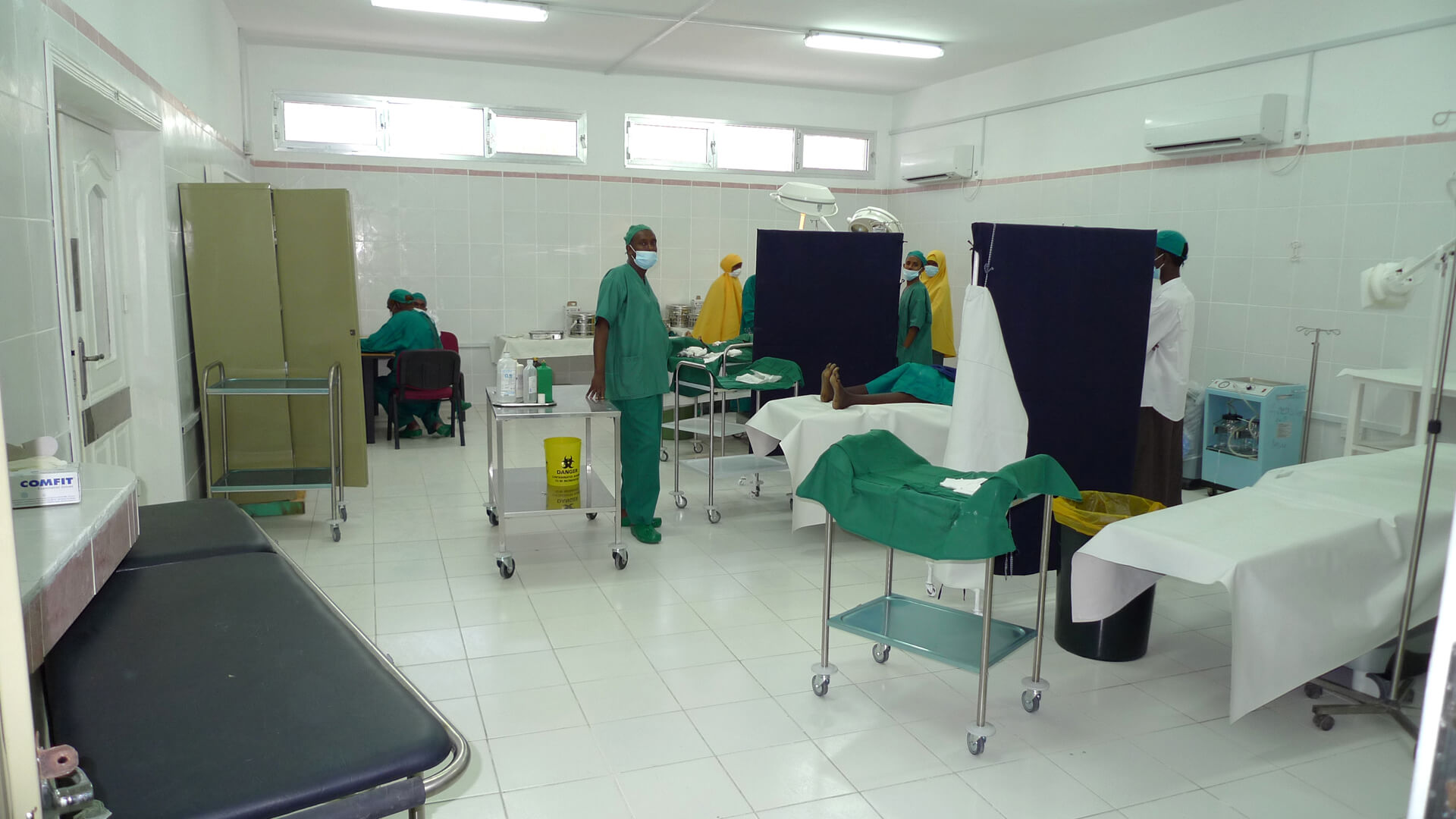
In many countries the Red Cross and Red Crescent societies are the main front line humanitarian responders, with 13 million-plus staff and volunteers around the world. I work with the ICRC, the oldest component of the International Red Cross and Red Crescent movement, a three-time Nobel Peace Prize Laureate with a mandate to protect the lives and dignity of victims of international armed conflicts and other situations of violence, and to provide them with assistance. More than 20 thousand ICRC staff in over 80 countries are providing healthcare for those affected by armed conflicts, securing humane treatment and conditions in detention, providing protection and care for civil populations, and taking other actions to address the effects of armed conflicts.
At the end of March, the ICRC launched a coordinated appeal with the International Red Cross and Red Crescent movement for resources to help the world’s most vulnerable communities halt the spread of the C19 pandemic and recover from its effects. Since the beginning of the pandemic, the ICRC has been directly engaged in life-saving services and support activities in places of armed conflict by supporting medical facilities and hospitals, assisting management of the dead, and providing medical response in places of detention, where people in overcrowded conditions are particularly at risk.
South Sudan, 2018. Photo: Mari Aftret Mortvedt, courtesy of ICRC.

As we have seen, high-income countries with well-functioning and robust healthcare infrastructures have been struggling to respond to C19’s direct effects. NY looked bad at the time of this webinar, but despite what has been going on there, NY has been a center of an international and multisector collaboration to overcome the crisis–foreign governments, cities, NGOs, and manufacturers have mobilized; ventilators and PPEs have crossed international lines to fill resource gaps. In war zones, non-government-controlled areas, and blockaded territories, that’s not going to happen. And what is important to grasp here is that C19 in these areas is an extra layer of complexity that comes on top of major risks from conflict, poverty, climate change, epidemics–HIV, TB, malaria–and more. And none of these stressors will stop with C19.
Ceará, Fortaleza, Brazil, 2020. Photo: Camila Almeida, courtesy of ICRC.

We have been “flattening the curve” in order to relieve stress on healthcare systems in many high-income countries, but in fragile countries where healthcare systems have been crippled by war, contact tracing and “flattening the curve” are a pipedream. In some places where the ICRC has been working for years there were fewer than ten ventilators for the whole country at the beginning of the crisis. So relieve stress on what in these conditions? Pandemic preparedness activities need to be contextualized. The ICRC answer from the onset of the crisis has been to support this contextualization for vulnerable populations.
Hand washing before ICRC distributes supplies, including soap, bleach, water, and washing stations, to detention centers in Burkina Faso. Photo: Hamidou Ouedraogo, courtesy of ICRC.

Another challenge comes from lessons learned from Ebola in West Africa in 2014. Many people died because of the sudden disruption of services–patients with TB died in greater numbers than patients with Ebola, for instance. Now, commercial airlines are down, borders are closed, and the full-on competition for drugs and medical equipment might put low-income states in a very bad position. International health logistics and humanitarian diplomacy are key.
COVID-19 response is aided by lessons learned in fighting tuberculosis in detention facilities like this one in Manila, where conditions are favorable to spread of disease. Photo: Jes Aznar, courtesy of ICRC, 2020.

Beyond the public health emergency, C19 is also a social and economic crisis with high probability of being a multiple-wave and protracted crisis. The humanitarian and development systems as we know them will be stretched to assist vulnerable populations.
Two highlights of interest to this audience: first, with C19, “urban” resilience is back at the agenda of the humanitarian and development sectors, and second, it’s about the built environment. A lot of initiatives are connecting urban specialists with local governments and mayors as they deal with C19. There is an opportunity here for urban specialists to support more decision makers at the front line of the crisis. As for the built environment: the role of built environment specialists, notably in NGOs and the army in some places, has gained in China, Europe, and the US. More built environment specialists should integrate health and public health dimensions in their training and practice to become more relevant and assertive at a time of human high vulnerability at global scale.